A pterygium is more than just a pinkish patch on the white of your eye. It’s a growth that creeps from the conjunctiva - the thin membrane covering the sclera - and starts climbing onto the cornea. Think of it like a tiny wing of tissue, slowly moving toward your pupil. When it gets close enough, it can blur your vision, make your eyes feel gritty, and even make wearing contact lenses impossible. This isn’t rare. In places like Australia, nearly 1 in 5 adults over 40 have it. And if you live near the equator, spend a lot of time outdoors, or never wear sunglasses, your risk goes up fast.
Why the Sun Is the Main Culprit
Ultraviolet (UV) light doesn’t just burn your skin - it damages your eyes too. Every time you’re outside without protection, your eyes are absorbing UV radiation. Over years, this builds up. Studies show that people who live within 30 degrees of the equator have more than double the risk of developing pterygium compared to those farther north or south. That’s because UV levels are strongest near the equator, and reflected off sand, water, and snow. A 2021 study found that cumulative UV exposure over 15,000 joules per square meter raises your risk by 78%. That’s roughly the amount you’d get from 3 hours of daily sun exposure over 10 years.
It’s not just about sunny days. Even on cloudy days, up to 80% of UV rays still get through. And UV exposure adds up silently. You might not notice it while you’re gardening, fishing, surfing, or driving. But over time, the tissue on the surface of your eye starts to change. Blood vessels grow, and the conjunctiva thickens into that triangular, fleshy bump you can see in the mirror. Most pterygia start on the nasal side of the eye - the side closest to your nose - because that’s where sunlight hits directly when you’re looking forward.
How It Progresses - And When to Worry
Not all pterygia grow. Some stay small and never cause trouble. Others creep slowly - about 0.5 to 2 millimeters per year - until they cover part of the cornea. Once it reaches the pupil, vision gets blurry. It can also cause astigmatism by changing the shape of the cornea. You might notice your eyes feeling dry, red, or irritated, like there’s sand in them. Contact lenses become uncomfortable. Some people develop double vision if the growth pulls on the cornea unevenly.
Doctors diagnose it with a simple slit-lamp exam. No blood tests. No scans. Just a bright light and a magnifying lens. The device lets them see the exact size, shape, and how far the growth has traveled onto the cornea. A pterygium under 1 millimeter wide is usually monitored. Once it’s over 3 millimeters and nearing the pupil, doctors start talking about treatment.
Pterygium vs. Pinguecula - What’s the Difference?
Many people confuse pterygium with pinguecula. They look similar - both are yellowish or pinkish bumps on the white of the eye. But here’s the key difference: a pinguecula stays on the conjunctiva. It never crosses onto the cornea. A pterygium does. That’s why one is mostly a cosmetic issue, and the other can affect vision. Pinguecula is more common - about 70% of outdoor workers in tropical areas have it. But only about 30% of those same people develop pterygium. The good news? Pinguecula rarely needs treatment. Pterygium might.
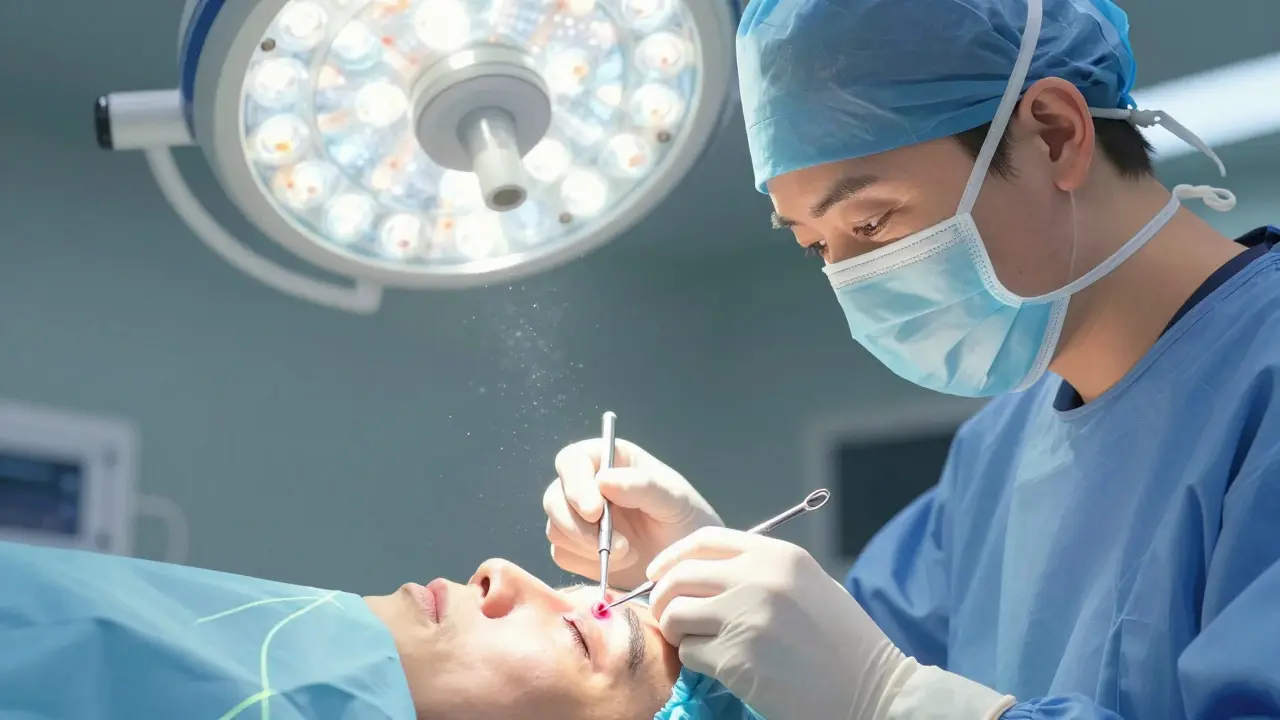
Surgical Options - What Actually Works
If your pterygium is blocking your vision or causing constant irritation, surgery is the only way to remove it. But here’s the catch: removing it isn’t the end of the story. Without the right technique, it comes back. In fact, traditional removal alone has a 30-40% recurrence rate. That’s why modern surgery isn’t just about cutting it out.
The most effective method today is conjunctival autograft. Here’s how it works: the surgeon removes the pterygium, then takes a tiny piece of healthy conjunctiva from another part of your eye - usually near the top - and stitches it over the bare spot. It’s like patching a hole with your own tissue. This reduces recurrence to just 8-10%. Many surgeons also use a drug called mitomycin C during surgery. It’s applied briefly to the eye’s surface to stop abnormal cells from regrowing. When combined with the autograft, recurrence drops even further - to about 5%.
Another newer option gaining traction is amniotic membrane transplantation. This uses tissue from the placenta - donated, sterilized, and safe. It acts like a biological bandage, calming inflammation and helping the eye heal naturally. European guidelines now recommend it as first-line treatment for recurrent pterygium, with success rates over 90% in preventing regrowth.
There’s also emerging research on laser-assisted removal and topical rapamycin. The FDA approved a new lubricant called OcuGel Plus in March 2023 specifically for post-surgery healing. Clinical trials showed it reduced dryness and discomfort 32% more than regular artificial tears. And a Phase II trial for rapamycin eye drops showed a 67% drop in recurrence at one year. These aren’t standard yet, but they’re coming fast.
What Recovery Looks Like
Surgery takes about 30-40 minutes and is done under local anesthesia. You’re awake but feel no pain. Most people go home the same day. Recovery isn’t quick, though. Your eye will be red, swollen, and sensitive for 2-3 weeks. You’ll need steroid eye drops for 4-6 weeks to prevent inflammation. Some patients say the drops are harder to stick with than the surgery itself. You can’t rub your eye. You’ll need to wear a shield at night for the first week. Most return to work in 3-5 days, but avoid swimming, dusty environments, and direct sun for at least a month.
Patients who get surgery report high satisfaction: 87% say their irritation is gone, and 65% notice immediate vision improvement. But 42% complain about lingering discomfort, and 37% are bothered by how red their eye looks during healing. That’s normal - it fades over time.

Prevention - Your Best Defense
The best treatment is no treatment. If you’re at risk - you live near the equator, work outdoors, or spend hours in the sun - prevention is simple:
- Wear UV-blocking sunglasses every day. Look for labels that say “UV400” or “blocks 99-100% of UVA and UVB.” ANSI Z80.3-2020 is the standard to check for.
- Use a wide-brimmed hat. It cuts UV exposure to your eyes by up to 50%.
- Don’t wait for a sunny day. UV levels above 3.0 require protection. That happens over 200 days a year even in places like Portland.
- Check your eyes annually. If you have a small bump, get it measured. Early detection means you can stop it before it grows.
One Reddit user, ‘OutdoorPhotog,’ said their pterygium stopped growing after they started wearing UV sunglasses daily. Their doctor confirmed it during two annual check-ups. That’s the power of prevention.
Who’s Most at Risk?
Men are more likely to develop pterygium than women - about 3 men for every 2 women. Why? It’s likely tied to outdoor work. Construction, farming, fishing, and surfing all mean more sun exposure. People over 40 are at higher risk too, because damage builds over time. And while it’s global, 65% of cases happen between 30°N and 30°S latitude. Australia has the highest national rate at 23% among adults over 40. In the U.S., rates are lower but rising as more people spend time outdoors.
What’s Next for Pterygium Care?
The global market for pterygium treatment is growing fast - it’s expected to hit $1.89 billion by 2028. That’s because more people are being diagnosed, and better treatments are becoming available. But there’s a big gap. In rural areas of developing countries, only 12% of people have access to surgery. In cities in the U.S. or Europe, it’s 89%. That’s not just a medical issue - it’s an equity issue.
As the ozone layer continues to thin and outdoor lifestyles become more popular, pterygium is becoming a growing public health concern. The tools to stop it - sunglasses, hats, regular eye exams - are simple. But they’re not always used. The real challenge isn’t surgery. It’s awareness.
Can pterygium cause blindness?
No, pterygium doesn’t cause total blindness. But if it grows large enough to cover the pupil, it can significantly blur your vision and cause astigmatism. In rare cases, it can distort the cornea so much that you lose sharpness in your sight. That’s why early treatment matters - not to prevent blindness, but to preserve clear vision.
Is pterygium cancerous?
No, pterygium is not cancerous. It’s a benign, noncancerous growth. It won’t spread to other parts of your body. But because it can look similar to rare eye cancers, doctors always check it carefully with a slit-lamp exam to be sure.
Can pterygium come back after surgery?
Yes, it can. Without advanced techniques, recurrence rates are 30-40%. But with conjunctival autograft and mitomycin C, that drops to 5-10%. Amniotic membrane transplants have even lower recurrence - under 10%. The key is the method used, not just the surgery itself.
Do I need surgery if my pterygium isn’t bothering me?
No. If your pterygium isn’t affecting your vision or causing discomfort, doctors usually recommend monitoring it instead. Use sunglasses and lubricating eye drops to manage dryness. Surgery is only considered if it grows toward the pupil, causes blurry vision, or makes contact lenses uncomfortable.
How can I tell if my pterygium is getting worse?
Watch for changes: increased redness, more visible blood vessels, the growth getting thicker or wider, or feeling like something is constantly in your eye. If you notice your vision becoming blurry - especially when looking straight ahead - that’s a sign it’s reaching the cornea. Make an appointment with your eye doctor for a measurement check.



8 Comments
Chris Crosson March 24, 2026 AT 18:56
I've been surfing for over 20 years and never wore proper sunglasses until last year. My left eye started getting that pinkish bump near the nose - scary stuff. Got it checked, and sure enough, early stage pterygium. Started wearing UV400 shades daily, and the redness has already faded. No surgery needed yet, but I’m not taking chances. Prevention really is the only real win here.
Also, hats. Don’t sleep on a wide-brimmed hat. It’s not just for fashion - it cuts UV exposure by half. Game changer.
Kevin Siewe March 26, 2026 AT 02:45
For anyone considering surgery - don’t rush it. If it’s not blocking vision or causing constant irritation, watchful waiting is totally fine. I had a small one for five years. My doctor monitored it with annual slit-lamp photos. It barely moved. I used preservative-free artificial tears twice a day and wore sunglasses even on cloudy days. No growth since. Surgery should be a last resort, not a first thought.
Also, those steroid drops post-op? Brutal. But necessary. Stick with them. I skipped a few days and regretted it.
Elaine Parra March 26, 2026 AT 10:50
Let’s be real - this whole thing is just another way for big ophthalmology to profit. You think they care about your vision? They care about the $1.89 billion market. Amniotic membrane transplants? That’s a luxury product. Most people can’t afford it. Meanwhile, you tell us to just wear sunglasses - like we all have the money or access to quality UV-blocking gear. This isn’t healthcare - it’s a capitalist scam wrapped in science-speak.
Chris Farley March 27, 2026 AT 22:50
Oh wow, so now we’re blaming the sun for eye problems? Next they’ll say breathing causes lung cancer. UV exposure? That’s natural. Your body adapts. If you’re getting pterygium from being outside, maybe you’re just weak. I’ve worked construction in Arizona for 30 years. No sunglasses. No hat. No surgery. Just toughed it out. People today are too soft. This isn’t a disease - it’s a character test.
Anil Arekar March 28, 2026 AT 13:18
As someone from India who has seen this condition in rural communities, I must emphasize the equity gap mentioned in the article. In villages, many laborers - fishermen, farmers - develop large pterygia because they cannot afford even basic UV-blocking sunglasses. Local clinics rarely have slit-lamp machines. I have volunteered with eye camps where we distributed recycled, certified UV400 sunglasses. A simple act, but it changed lives. Awareness and access are not luxuries - they are necessities. Let us not forget that medical advancement means nothing if it does not reach those who need it most.
Rama Rish March 28, 2026 AT 15:14
i had one in my left eye 5 years ago. just started wearing shades and it stopped growing. no surgery. no drama. simple. wear sunnies. always.
Mihir Patel March 29, 2026 AT 18:35
so i got my pterygium removed last year with the amniotic membrane thingy. best decision ever. the recovery was wild - red for weeks, felt like sandpaper in my eye for a bit. but now? crystal clear. no more gritty feeling. i even started surfing again. the docs said 90% success rate and i’m living proof. also, the drops were annoying but worth it. if you’re thinking about it - just do it. your future self will thank you.
Linda Foster March 31, 2026 AT 10:19
The distinction between pterygium and pinguecula is critical, and I appreciate the clarity provided in this post. As an ophthalmic technician, I have observed that many patients conflate the two, leading to unnecessary anxiety. Pinguecula, while visually concerning, is a benign, degenerative change of the conjunctiva, often associated with chronic exposure to wind and dust. It rarely progresses and seldom requires intervention. Pterygium, by contrast, is a proliferative condition with potential visual consequences. Accurate diagnosis through slit-lamp examination remains the gold standard, and patient education must be grounded in this precision. Prevention, as noted, remains the most effective and equitable strategy.